Prescription Drug and Addiction Myths
Xanax, Adderall, and Zoloft are as addictive as Percocet and Vicodin
We hear regularly about the addictive surge occurring with opioid painkillers such as Vicodin, Percocet, and Oxycontin—a recent victim of which was Prince. In fact, most people who take these drugs regularly do not become addicted—quite a small percentage do, in fact.
In the meantime, quite a few—just as many—become addicted to such popular drugs as Xanax, Adderall, and Zoloft. But, for reasons we will explain, these addictions are ignored.
The Life Process Program is able to deal with the equivalent addictiveness of these substances because it approaches addiction as a process whereby a person becomes enmeshed in an experience, one that combines physical, emotional, and cognitive elements. If the person finds that a substance produces an experience in which they can immerse themelves, then they stand a chance of becoming addicted to it.
Let’s review these leading addictive pharmaceutical substances.
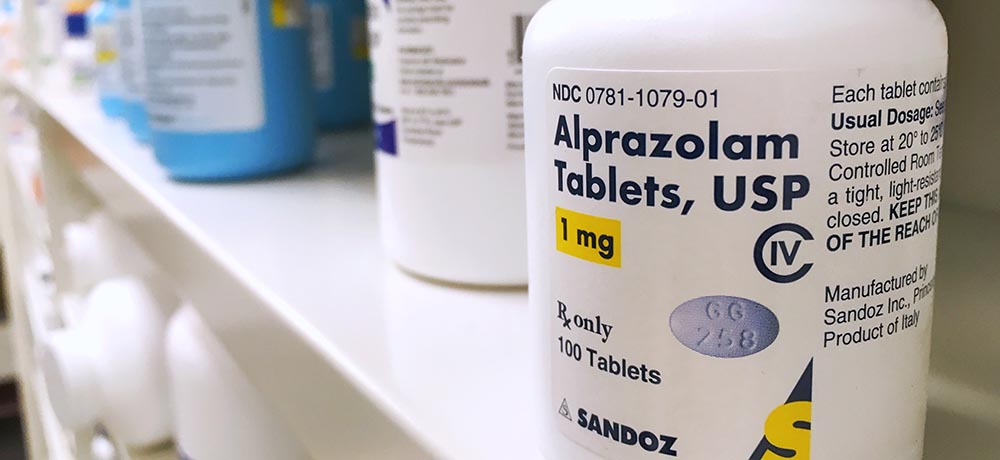
- Xanax is a benzodiazapine, commonly called a tranquilizer, used to treat anxiety. We have for some time been aware of the addictive properties of benzos (as they are called)—Barbara Gordon wrote the 1979 bestseller “I’m Dancing as Fast as I Can” about her tranquilizer addiction, one that she couldn’t shake despite repeated hospitalizations.
Once tranquilizers—the Rolling Stones’ “Mother’s Little Helper”—had a slightly humorous image as the secret resort of the harried housewife, No more. Benzodiazapine deaths are rampant, rising as fast as—and sometimes more rapidly than—deaths due to opioids (with which they are often combined).
Between 1996 and 2013 benzodiazapine deaths quintupled—from .6 to 3.0 per 100,000 adults annually. These now comprise 30 percent of all drug deaths, even though far fewer people use tranquilizers than painkillers (which almost a third of American take in a given year). In part the failure to sound alarm bells about prescription drugs such as Xanax is due to the greater attention that opioid deaths have received. Despite the “benzodiazepine crisis,” people have a hard time accepting the lethal potential of mother’s little helper.
- Zoloft is perhaps the best know SSRI antidepressant, used to treat depression, obsessive-compulsive disorder, social anxiety, panic disorder, et al. For some time, the myth has been spread that people don’t suffer withdrawal (i.e., become addicted) to antidepressants. Again, this is due to the fallacy that only a single, specific type of drug, the opioids, is chemically capable of producing addiction.
But antidepressant users are becoming addicted—and suffering withdrawal—in droves, as revealed in an April article in the New York Times, “Many People Taking Antidepressants Discover They Cannot Quit”—i.e., they are addicted. This is striking because more and more people in the U.S. take antidepressants such as Zoloft, and take them for considerable lengths of time: “Some 15.5 million Americans have been taking the medications for at least five years. The rate has almost doubled since 2010, and more than tripled since 2000.”
- Adderall is an amphetamine, a stimulant, used to treat ADHD (attention deficit disorder) in children and teens; its long-acting counterpart is Concerta. As Columbia University psychology and psychiatry professor Carl Hart notes, the chemical structure of Adderall is very similar to that of methamphetamines, as are its effects in sufficient doses.
Pundits are now referring to millennials as “Generation Adderall”: “In the 1990s, an estimated 3 to 5 percent of school-age American children were believed to have ADHD, according to the Centers for Disease Control and Prevention; by 2013, that figure was 11 percent. It continues to rise. And the increase in diagnoses has been followed by an increase in prescriptions. In 1990, 600,000 children were on stimulants. . . By 2013, 3.5 million were on stimulants,” usually Adderall.
The author of Generation Adderall described his own drive to consume the drug after he “became one of the millions of Americans to be prescribed a stimulant medication. . . During the decade I was entangled with Adderall”:
I would open other people’s medicine cabinets, root through trash cans where I had previously disposed of pills, write friends’ college essays for barter. Once, while living in New Hampshire, I skipped a day of work to drive three hours each way to the health clinic where my prescription was still on file.
Sound like addiction to you? Then why don’t people recognize it? When not only the public, but addiction “experts,” are convinced that only opiates are addictive, they fail to notice the obvious symptoms of addiction to other prescription drugs displayed all around them. We might call it “addictive denial.”
In the Life Process Program, we recognize that the cure for addiction is for people to, first, recognize their own power to overcome addiction. Second in the LPP process for overcoming addiction is helping people to connect directly to the satisfactions they are able to generate through normal life activities, whether work and study, friends and family, or values and purpose in their lives.
There is no magic to overcoming addiction—just as there is no magical potion, such as the opioids, that causes addiction. Addiction and recovery involve the straightforward, although rarely simple, matter of engaging in life, as opposed to hiding out from it, no matter what the chemical agent involved is.






My daughter nearly killed herself with Xanax while she was with an out patient drug treatment program. I will have to say that bunch caused more problems than they solved.